T cells are highly specialized lymphocytes that play a critical role in the cell-mediated arm of the adaptive immune response. Without them, our bodies would not be able to successfully fight off viral infections or scour tissues to eliminate some pre-cancerous cells.
 |
Explore curated antibody sampler kits from CST: • T Cell Signaling Antibody Sampler Kit #14541 • Mouse Immune Cell Phenotyping IHC Antibody Sampler Kit #37495 • Human Immune Cell Phenotyping IHC Antibody Sampler Kit #62714 |
The Role of T Cells
Through the specific activation of cell surface signaling receptors, certain T cells can:
- Exert cytotoxic effects to kill and remove perceived threats—like virally infected cells and cancer cells,
- Secrete cytokines to influence and guide the actions of other immune cells, and
- Distinguish foreign pathogenic antigens from self-antigens—thus providing tolerance by preventing immune cells from mounting an inappropriate autoimmune response to the body’s own cells.
In recent years, researchers have sought to exploit the actions of T cells via genetic engineering, with the goal of tailoring their effector cell functions to target and remove cancer cells. These essential roles in immune protection and their potential for therapeutic use underscore why it is important to fully understand the signaling cascades that guide T cell behavior.
T cells, which are identified by the expression of CD3 on their cell surface, arise from lymphoid progenitor cells which, in turn, are derived from hematopoietic stem cells in the bone marrow. Upon migration to the thymus through the bloodstream, T cells differentiate following the rearrangement of the T cell receptor (TCR) gene.
Although there are many types of T cells, the main types include CD4+ helper T cells, CD8+ cytotoxic T cells, or natural killer T (NKT) cells. The specific roles of each of these types of T cells are regulated by the activation of their cell surface receptors and costimulatory molecules. For example, helper T cells respond to peptide antigens bound to MHC class II molecules on the surface of antigen-presenting cells.
These signals induce the helper T cells to rapidly proliferate and secrete cytokines, which in turn, modulate the immune response by activating cytotoxic T cells and stimulating B cells to secrete antibodies. Similarly, cytotoxic T cells are activated when they recognize antigen-bound MHC class I molecules on the surface of infected cells or tumor cells. This triggers T cells to kill the affected cell by inducing apoptosis. NKT cells express an invariant T cell receptor, and unlike conventional T cells, can be stimulated to respond to pro-inflammatory cytokines in the absence of primary antigen activation to engage in T cell effector functions—including enhanced proliferation, cytokine release, and cell-mediated cytotoxicity. Although NKT cells have some similarity to other T cells, they share more characteristics with cells of the innate immune system.
Activation of Cytotoxic T-Cell Phenotypes
How do interactions at the surface of the T cell lead to rapid activation and expression of the cytotoxic phenotypes listed above? A series of events take place in order to fully activate the immune response:
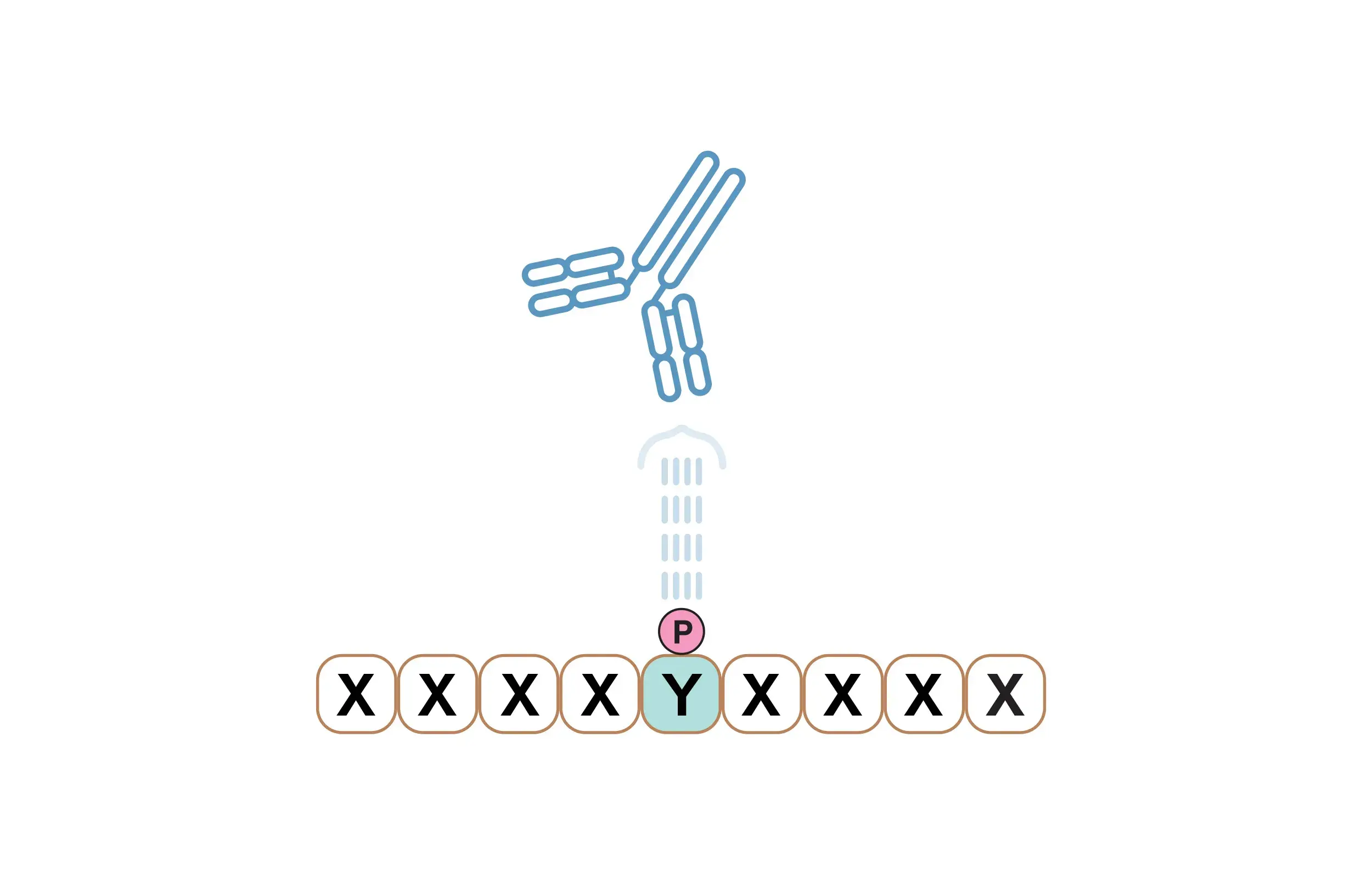
- Antigen binding to the TCR results in the intracellular phosphorylation (by a member of the Src kinase family called Lck) of a motif on the cytosolic tail of the TCR/CD3 complex, called the immunoreceptor based activation motif (ITAMs).
- Zeta-chain associated protein kinase 70 (Zap-70) is recruited to phosphorylate its substrate SLP-76.
- The association of downstream adaptor proteins—including Vav, NCK, GADS, and interleukin-2 inducible T cell kinase (Itk)—is promoted.
- Subsequent signaling via downstream pathways including PKCq and MAPK/Erk coordinate with parallel signaling through pathways like PI3K/AKT—activated by costimulatory receptors including CD28 and CD45.
- This activation induces the translocation of key transcription factors to the nucleus and upregulation of genes associated with the appropriate T cell effector phenotypes.
- Transcription factors including NFAT, NF-kB, Fos, and Jun mediate changes in gene expression in response to TCR activation.
Taken together, the combined activation of T cell surface receptors ultimately modulates the immune cell response.
Additional Resources
Explore additional blog posts about T cells and the immune response:




/Binary_oasis_Blog%20Header.webp)
