The tuberous sclerosis complex (TSC) is a tumor suppressor composed of TSC1 and TSC2.24,25 The TSC affects cellular metabolism by regulating transcription or, alternatively, autophagy.25 Under adverse conditions, AMP-activated protein kinase (AMPK) phosphorylates TSC2 and promotes the formation of the TSC1-TSC2 complex, which then inhibits mTORC1 activity (24-25). AKT-mediated phosphorylation inhibits TSC2 and releases that inhibition to activate mTORC1.1,25
The continuous activation of mTORC1 results in the dephosphorylation of Akt, which suppresses the feedback of mTORC1.25 In this way, mTORC1 is both a downstream activation target of Akt as well as a pathway inhibitor via negative feedback effects on Akt.1,24,25
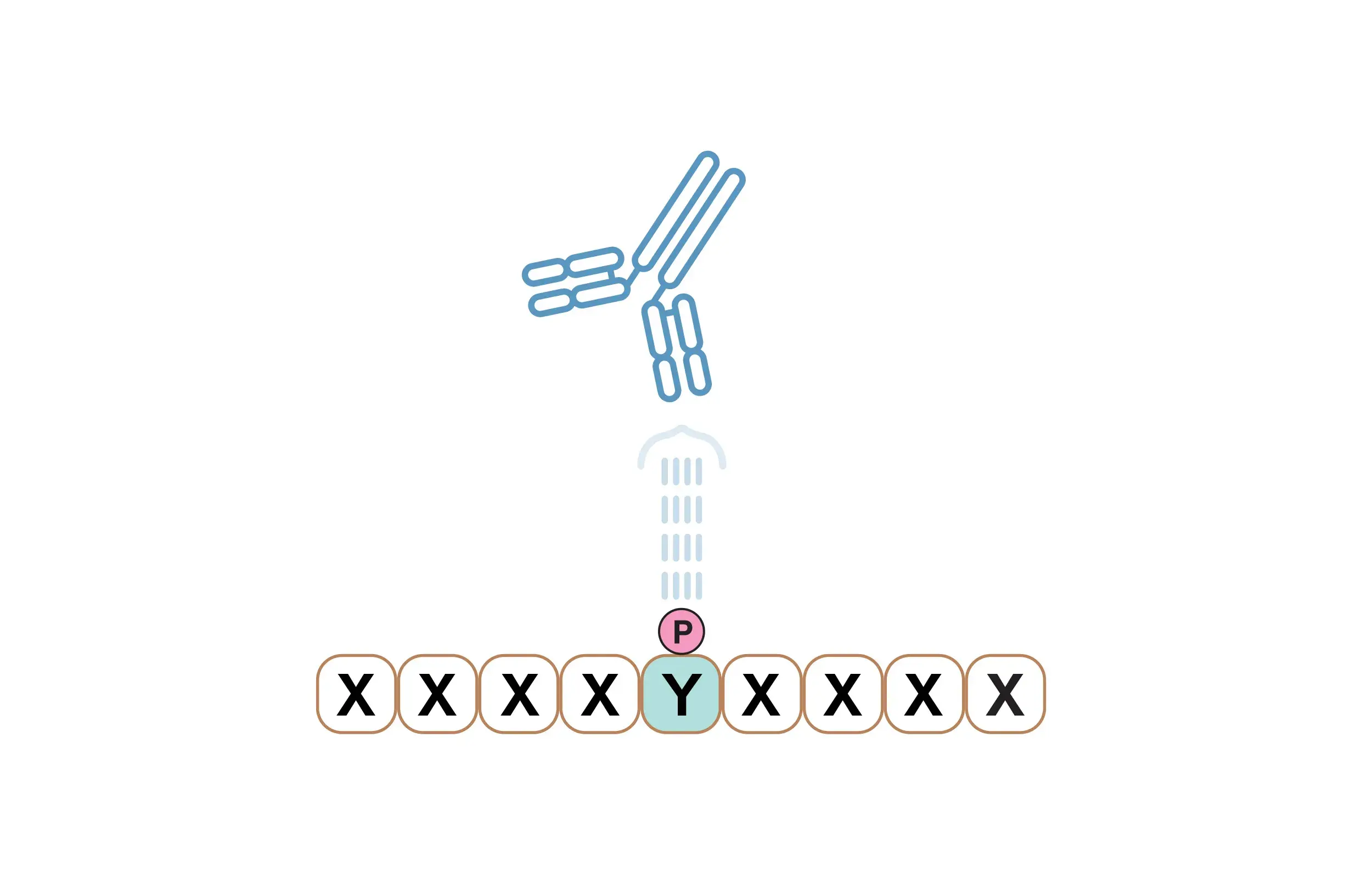
Plasma cells/plasmocytes secrete protective antibodies against infectious agents but they also produce pathogenic antibodies (autoantibodies) that target the body’s cells in autoimmune diseases, such as systemic lupus erythematosus (SLE).26. mTORC1 overactivation can lead to increased plasmocyte and autoantibody production, possibly enhancing pathogenesis.24-26
Clues for Solving the PI3K/Akt Puzzle
Given the broad reach of PI3K/Akt signaling, it is not surprising that Akt plays a central yet diverse role in the response of various cell types and tissues to a wide range of stimuli.1-2 However, it is important to keep in mind that the PI3K/Akt pathway is an integral part of larger signaling networks and all signaling is contextual and dynamic. In terms of pathology, research scientists and medical professionals are playing a signaling version of the board game Clue. Every day, they're asking questions like: Who’s the pathological culprit? Which target signaling mechanism(s) were used? In which cells or organ systems?
As the race to unravel complex signaling networks continues, scientists continually need research tools to help. This is where Cell Signaling Technology fits into the puzzle. Our company mission is to make the most relevant, useful, and reproducible products for cancer and translational research. We strive to provide reliable signaling tools to the scientific community in order to help researchers manage and manipulate these signaling networks to hopefully one day treat the diseases that affect so many of the loved ones in our lives.
Explore PI3K/AKT/MAPK signaling resources.
20-CEP-97405
References
- Manning BD, Toker A. AKT/PKB Signaling: Navigating the Network. Cell. 2017 Apr 20; 169(3): 381–405.
- Martini, Miriam & De Santis, Maria & Braccini, Laura & Gulluni, Federico & Hirsch, Emilio. (2014). PI3K/AKT Signaling pathway and cancer: An updated review. Annals of medicine. 46. 1-12
- Feng Y, Spezia M, Huang S, Yuan C, Zeng Z, Zhang L, Ji X, Liu W, Huang B, Luo W, Liu B, Lei Y, Du S, Vuppalapati A, Luu HH, Haydon RC, He TC, Ren G. Breast cancer development and progression: Risk factors, cancer stem cells, signaling pathways, genomics, and molecular pathogenesis. Genes Dis. 2018 May 12;5(2):77-106.
- Yip, C.C. and Ottensmeyer, P. (2003) J Biol Chem 278, 27329-32.
- Antonino Belfiore, Francesco Frasca, Giuseppe Pandini, Laura Sciacca, Riccardo Vigneri, Insulin Receptor Isoforms and Insulin Receptor/Insulin-Like Growth Factor Receptor Hybrids in Physiology and Disease, Endocrine Reviews, Volume 30, Issue 6, 1 October 2009, Pages 586–623.
- Belfiore A, Malaguarnera R, Vella V, Lawrence MC, Sciacca L, Frasca F, Morrione A, Vigneri Insulin Receptor Isoforms in Physiology and Disease: An Updated View. Endocr Rev. 2017 Oct 1;38(5):379-431.
- Escribano O, Beneit N, Rubio-Longás C, López-Pastor AR, Gómez-Hernández A. The Role of Insulin Receptor Isoforms in Diabetes and Its Metabolic and Vascular Complications. J Diabetes Res. 2017;2017:1403206.
- Lizcano J. M. Alessi D. R. (2002) The insulin signaling pathway. Curr Biol. 12, 236-238.
- Alam F, Islam MA, Khalil MI, Gan SH. Metabolic Control of Type 2 Diabetes by Targeting the GLUT4 Glucose Transporter: Intervention Approaches. Curr Pharm Des. 2016;22(20):3034-3049.
- Mukohara T. PI3K mutations in breast cancer: prognostic and therapeutic implications. Breast Cancer (Dove Med Press). 2015;7:111‐123.
- Nwabo Kamdje A.H., Seke Etet P.F., Vecchio L., Muller J.M., Krampera M., Lukong K.E. Signaling pathways in breast cancer: therapeutic targeting of the microenvironment. Cell Signal. 2014;26(12):2843–2856.
- Thorpe LM,Yuzugullu H, Zhao JJ. PI3K in cancer: divergent roles of isoforms, modes of activation and therapeutic targeting. Nat Rev Cancer. 2015; 15: 7-24.
- Batlevi CL, Younes A. Revival of PI3K inhibitors in non-Hodgkin’s lymphoma. Annals of Oncology. 2017; 28(9): 2047-2049.
- Curran E, Smith SM. Phosphoinositide 3-kinase inhibitors in lymphoma. Curr Opin Oncol. 2014 Sep;26(5):469-75.
- Schatz, J.H. Targeting the PI3K/AKT/mTOR Pathway in Non-Hodgkin’s Lymphoma: Results, Biology, and Development Strategies. Curr Oncol Rep 13, 398 (2011).
- Blachly, J.S. and Baiocchi, R.A. (2014), Targeting PI3‐kinase (PI3K), AKT and mTOR axis in lymphoma. Br J Haematol, 167: 19-32.
- Lawrence J, Nho R. The Role of the Mammalian Target of Rapamycin (mTOR) in Pulmonary Fibrosis. Int J Mol Sci. 2018 Mar 8;19(3):778.
- Lei P, Ayton S, Bush AI, Adlard PA. GSK-3 in Neurodegenerative Diseases. Int J Alzheimers Dis. 2011:189-246.
- Kockeritz L, Doble B, Patel S, Woodgett JR. Glycogen synthase kinase-3--an overview of an over-achieving protein kinase. Curr Drug Targets. 2006 Nov; 7(11):1377-88.
- Hritzo Ahye MK, Golding A. Cytoplasmic FOXO1 identifies a novel disease-activity associated B cell phenotype in SLE Lupus Science & Medicine 2018;5:e000296.
- Lu M, Xu W, Gao B, Xiong S. Blunting Autoantigen-induced FOXO3a Protein Phosphorylation and Degradation Is a Novel Pathway of Glucocorticoids for the Treatment of Systemic Lupus Erythematosus. J Biol Chem. 2016 Sep 16;291(38):19900-12.
- Lin L, Hron JD, and Peng SL. (2004). Regulation of NF-κB, Th activation, and autoinflammation by the forkhead transcription factor Foxo3a. Immunity 21, 203–213.
- Zhou W, Cao Q, Peng Y, Zhang QJ, Castrillon DH, DePinho RA, and Liu ZP. (2009) FoxO4 inhibits NF-κB and protects mice against colonic injury and inflammation. Gastroenterology 137, 1403–1414.
- He J, Ma J, Ren b, Liu A. Advances in systemic lupus erythematosus pathogenesis via mTOR signaling pathway. Semin Arthritis Rheum. 2020 Apr;50(2):314-320.
- Stylianou K, I Petrakis, V Mavroeidi, S Stratakis, E Vardaki, K Perakis, et al. The PI3K/Akt/mTOR pathway is activated in murine lupus nephritis and downregulated by rapamycin. Nephrol Dialysis Transplant, 26 (2) (2011), pp. 498-508.
- Malkiel S, Barlev AN, Atisha-Fregoso Y, Suurmond J, Diamond B. Plasma Cell Differentiation Pathways in Systemic Lupus Erythematosus. Front Immunol. 2018 Mar 5;9:427.








/Binary_oasis_Blog%20Header.webp)
